Welcome to ARChoices in Homecare, a Medicaid program that includes home and community-based services for adults ages 21 through 64 with a physical disability and seniors age 65 or older.
These services can offer help doing everyday activities that you may no longer be able to do for yourself like bathing, dressing, getting around your home, preparing meals, or doing household chores.
ARChoices in Homecare Brochure
ARChoices in Homecare Brochure (Spanish Version)
DHS RN County and Contact Information
Personal Care Referral Form
VIDEO: Learn more about adult day care
Am I Eligible?
To qualify for for ARChoices in Homecare, you must be:
•Age 21 through 64 with a physical disability OR
•Age 65 and older
AND
•Meet established financial criteria.
•Meet nursing home admission criteria at the intermediate level.
•Have a need for at least one of the available services
What Services are Available?
Attendant Care – When someone helps you do the things like get out of bed, take a bath, get dressed, fix and eat meals, or use the bathroom
Home-Delivered Meals – Nutritious meals that can be delivered fresh each day or frozen for weekends.
Personal Emergency Response System (PERS) – A call button you can use to get help in an emergency.
Adult Day Services – A place provides supervised care and activities during the day. For more information, please call 1-866-801-3435 from 8 a.m. to 4 p.m. Monday – Friday.
Adult Day Health Services – a place that provides skilled nursing, supervised care, and activities during the day.
Facility-Based Respite Care – Short Stays in a facility so your caregiver can go on vacation.
In-Home Respite Care – Someone to stay with you in your home for a short time so your caregiver can get some rest.
Environmental Modifications – Changes to your home that will help you get around more easily and safely like grab bars or a wheelchair ramp.
Court-Ordered Information
Before 2013, DHS used a paper form to determine eligibility for the department’s home- and community-based Medicaid waiver services for adults with physical disabilities and the frail elderly. In 2013, DHS began to use the ArPath Assessment tool for determining eligibility only.
In January 2016, DHS combined two prior Medicaid waivers, known as Alternatives for Adults with Physical Disabilities (AAPD) and ElderChoices, into a single Medicaid waiver known as ARChoices. The Centers for Medicare and Medicaid Services (CMS) approved the ARChoices waiver with the understanding that DHS would begin to use an objective tool to allocate attendant care hours for beneficiaries. Upon approval of the ARChoices waiver, the prior waivers expired. DHS then began using this new tool, known as the Resource Utilization Groups (RUGs) methodology, in conjunction with the ArPath Assessment tool to determine the number of attendant care hours ARChoices beneficiaries receive.
On January 26, 2017, a group of seven (7) ARChoices beneficiaries filed a lawsuit in Pulaski County Circuit Court challenging the method by which DHS adopted the regulation authorizing use of the RUGs methodology, alleging that it did not provide sufficient details regarding RUGs during the rulemaking process. On February 7, 2017, the Court entered a temporary restraining order (TRO), providing “DHS is enjoined from conducting reassessments on Plaintiffs and reducing their Attendant Care hours under the RUGs system.”
On May 14, 2018, the Court ruled that DHS did not substantially comply with notice requirements when DHS adopted the RUGs methodology. Specifically, the Court found that the notice did not refer to the specific nature and significance of the change in assessment methodology. The Court ruled that DHS was barred from using the RUGs methodology to allocate attendant care hours for any beneficiary in the state until it properly promulgated the rule implementing use of the RUGs methodology. While DHS is appealing this ruling, the Court has ordered DHS to post some specific information to its website about ARChoices beneficiaries.
In an order dated June 25, 2018, the Court ordered DHS to “publish on its website … the number of persons it assessed and re-assessed for attendant care using registered nurses for every month before Jan. 1, 2016, when it began employing the RUGs methodology.” That information is below.
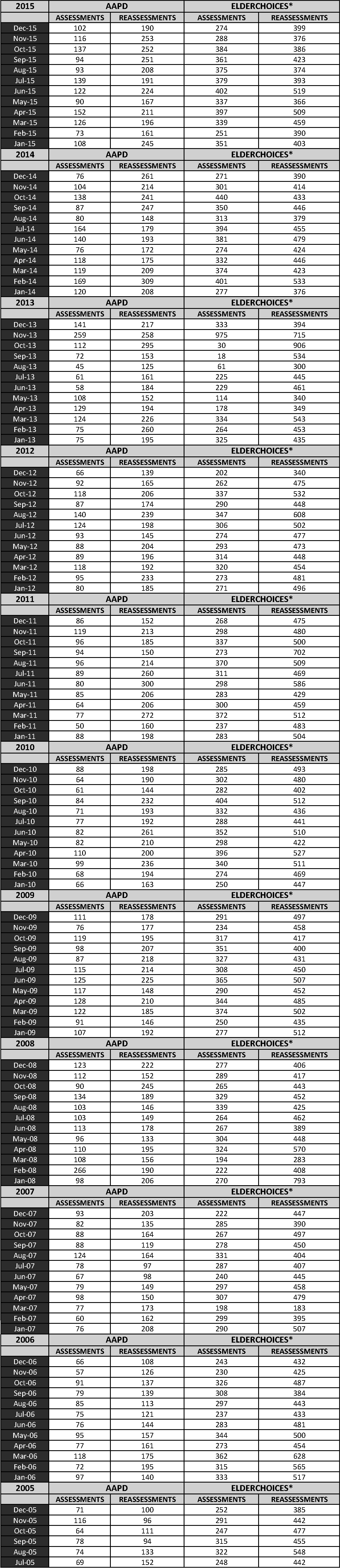
Attendant care services were provided only for AAPD clients. Attendant care was not an available service under ElderChoices, but some similar services were offered. The two programs combined on January 1, 2016, to form ARChoices, providing attendant care services to all clients.
Download PDF: Completed Assessments and Reassessments 2005-2015
In the June 25, 2018 order, the Court also ordered DHS to “publish on its website … the number of persons it has failed or refused to reassess each month since February 7, 2017….” On that date, the Judge wrote that DHS “is enjoined from conducting reassessments on Plaintiffs and reducing their Attendant Care hours under the RUGs system.” We have included numbers both for assessments and reassessments, even though the order only calls for reassessment numbers. These numbers reflect individuals for whom DHS failed or refused to perform an assessment or a reassessment between February 7, 2017, and June 25, 2018.
Pursuant to the Court’s Order of February 7, 2017, only the named plaintiffs were denied assessment or reassessment during the relevant time period. Other beneficiaries and potential beneficiaries may not have received an assessment or reassessment for reasons unrelated to this litigation, including without limitation that the client was deceased; the client could not be located; the client did not have a change of circumstance sufficient to warrant reassessment; the client requested their case to be closed; or the client was no longer financially eligible for the waiver.
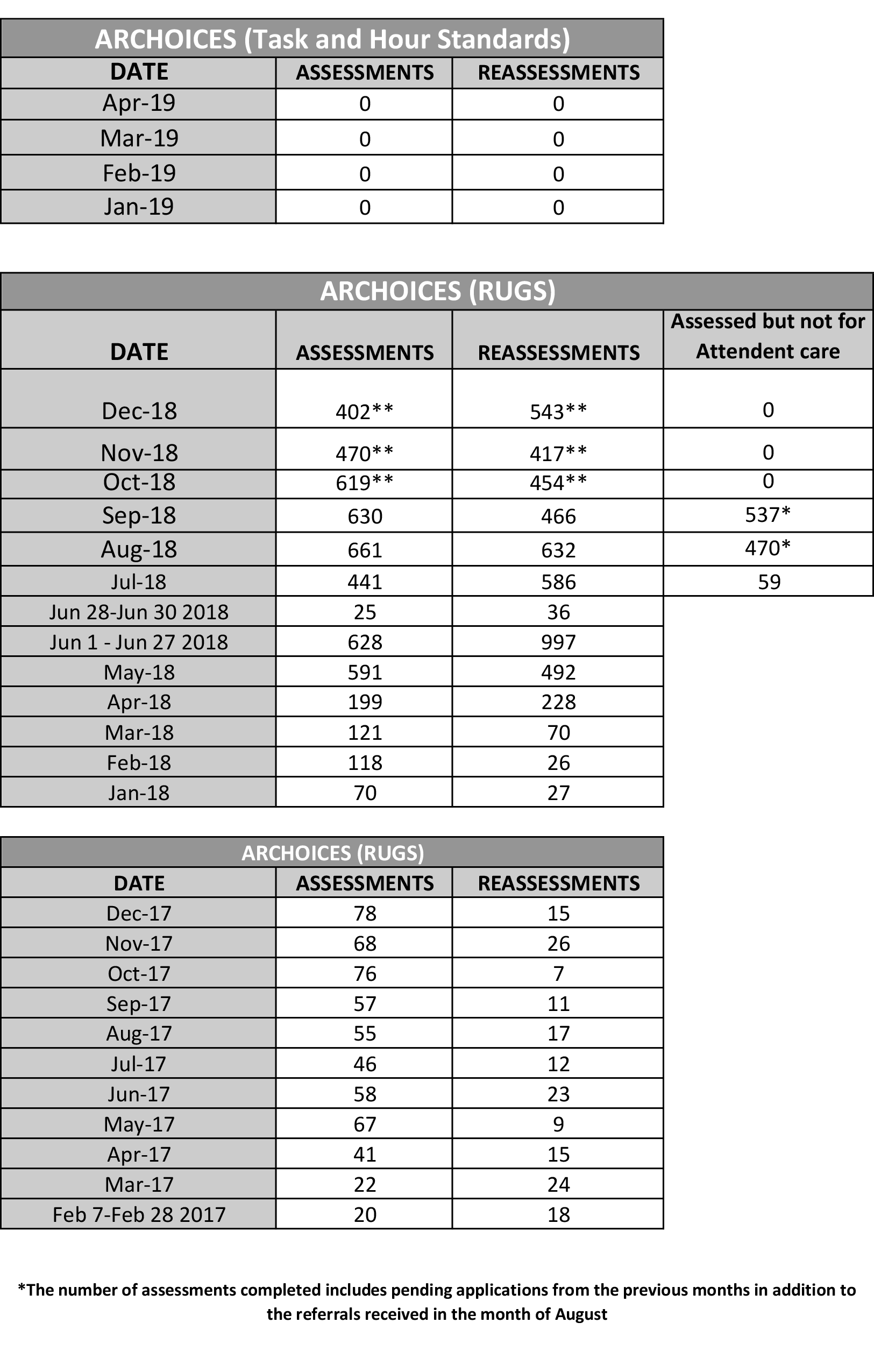
Download PDF: Assessments and Reassessments 2017-2019



